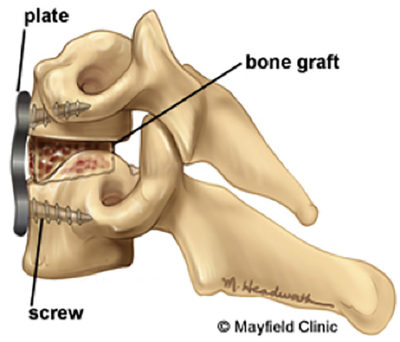
Anterior cervical fusion (ACF) is one of the most frequently performed spine procedures in the United States, providing a reliable solution for a spectrum of cervical‑spine disorders that compress the spinal cord or nerve roots. By accessing the cervical vertebrae from the front of the neck, the surgeon removes the offending disc, osteophyte, or ligamentous tissue and then stabilizes the segment with a bone graft or interbody cage, often supplemented with a plate and screws. The goal is to create a solid bony bridge that eliminates motion at the diseased level, thereby decompressing neural structures and restoring alignment. While the procedure has a long track record of success, it is not without potential downsides. Understanding both the benefits and the risks helps patients, families, and clinicians weigh whether ACF is the most appropriate intervention for a given condition.
Why Anterior Cervical Fusion Is Considered
- Targeted Decompression – Most cervical radiculopathy and myelopathy stem from a single or limited number of levels. The anterior route offers a direct line of sight to the disc‑space, uncovertebral joints, and posterior longitudinal ligament, allowing the surgeon to excise the pathological tissue with minimal disturbance to the posterior musculature and ligamentous complex.
- Immediate Stability – By inserting a structural graft or cage that bears load, the surgeon provides instant mechanical support. This reduces the reliance on postoperative immobilization devices such as cervical collars and encourages earlier mobilization.
- Correction of Sagittal Alignment – In cases of cervical kyphosis or loss of lordosis, the interbody device can be positioned to restore a natural curve, which has been linked to better long‑term functional outcomes and reduced strain on adjacent segments.
- High Fusion Rates – Modern techniques that combine autograft or allograft bone with biologic adjuncts (e.g., demineralized bone matrix, recombinant BMP) achieve fusion rates exceeding 90 % in most series, translating into durable symptom relief.
Because the procedure can address pain, neurological deficits, and deformity in a single operation, it remains a cornerstone of cervical spine surgery.
Core Benefits of Anterior Cervical Fusion
1. Pain Relief and Functional Recovery
The most immediate benefit reported by patients is a reduction in neck and arm pain. By eliminating the inflamed disc or osteophyte that irritates nerve roots, ACF often produces a rapid decline in radicular pain, sometimes within the first postoperative week. In myelopathic patients, the decompressional effect can halt disease progression and, in many cases, yield measurable improvements in gait, hand dexterity, and bladder function. A systematic review of over 3,000 patients demonstrated a mean visual‑analog‑scale (VAS) pain reduction of 5.5 points (on a 10‑point scale) and a 70 % improvement in the Neck Disability Index (NDI) at one‑year follow‑up.
2. Long‑Term Stability and Deformity Prevention
Fusion creates a solid bone bridge that eliminates pathological motion at the treated level. This stability protects against recurrent disc herniation and prevents the development of segmental instability—a frequent cause of chronic neck pain after discectomy alone. Furthermore, by preserving or restoring cervical lordosis, the surgery reduces the shear forces transmitted to adjacent vertebrae, decreasing the risk of subsequent deformity.
3. High Success Rate and Predictable Outcomes
Numerous prospective cohort studies have reported a 90–95 % rate of satisfactory outcomes (defined as ≥30 % improvement in pain scores or functional indices). The predictability stems from the procedure’s relatively straightforward anatomy, the ability to verify decompression intraoperatively, and the use of modern fixation devices that resist hardware loosening.
4. Short Hospital Stay and Early Return to Activity
Advances in peri‑operative care—such as minimally invasive approaches, multimodal analgesia, and early mobilization protocols—have shortened the average hospital stay to 1–2 days for most patients. Many individuals resume light activities within a week and return to full work duties (particularly non‑manual occupations) by 4–6 weeks, a timeline markedly faster than that of posterior fusion procedures.
5. Low Reoperation Rate When Properly Indicated
When performed on appropriately selected patients (single‑level disease, good bone quality, and absence of severe osteoporosis), ACF carries a relatively low reoperation rate—typically <5 % within five years. The most common cause for re‑intervention is adjacent‑segment degeneration (ASD), a phenomenon that also affects non‑surgical patients but can be mitigated by preserving overall cervical alignment.
Potential Risks and Complications
Every surgical intervention carries inherent risk, and anterior cervical fusion is no exception. Understanding the frequency, severity, and strategies for mitigation of these complications enables patients to make an informed decision.
1. Dysphagia (Swallowing Difficulty)
- Incidence: 5–30 % (transient), <2 % (persistent >6 months).
- Mechanism: Retraction of the esophagus and pharynx during surgery can cause edema, minor trauma, or postoperative scar formation.
- Management: Most cases resolve with a soft‑diet progression and anti‑inflammatory medication. Persistent dysphagia may require endoscopic evaluation or, rarely, surgical release of scar tissue.
2. Hoarseness and Recurrent Laryngeal Nerve (RLN) Injury
- Incidence: 1–5 % (temporary), <0.5 % (permanent).
- Mechanism: The RLN runs close to the anterior cervical spine; excessive retraction or thermal injury from electrocautery can impair vocal cord function.
- Management: Temporary hoarseness improves with voice therapy; permanent injury may necessitate otolaryngology referral and possible medialization procedures.
3. Infection
- Incidence: 0.5–2 % for superficial wound infection; deep‑space infection (e.g., discitis, mediastinitis) is <0.2 %.
- Risk Factors: Diabetes, smoking, prolonged operative time, and prior cervical surgery increase susceptibility.
- Management: Prompt intravenous antibiotics for early infections; surgical debridement may be required for deep infections.
4. Hardware‑Related Complications
- Plate or Screw Loosening: Occurs in <3 % of cases, often linked to poor bone quality or over‑loading of the construct.
- Cage Migration or Subsidence: Can cause recurrent neural compression. Modern cages with porous titanium or PEEK designs reduce this risk, yet subsidence rates of 5–10 % are still reported, especially in osteoporotic patients.
- Management: Revision surgery with hardware replacement or supplemental posterior fixation is sometimes needed.
5. Vascular Injury
- Incidence: Rare (<0.1 %).
- Mechanism: The carotid artery and vertebral artery lie laterally; inadvertent injury can cause catastrophic hemorrhage. Intra‑operative Doppler and meticulous dissection dramatically lower this risk.
6. Neurological Deterioration
- Incidence: <1 % for new or worsening motor/sensory deficits.
- Mechanism: Direct trauma to the spinal cord or nerve roots, or ischemia from prolonged retraction.
- Management: Intra‑operative neuro‑monitoring (somatosensory and motor evoked potentials) helps detect early changes, allowing immediate corrective actions. Post‑operative steroids are reserved for acute deficits.
7. Adjacent‑Segment Degeneration (ASD)
- Incidence: Radiographic changes in 20–40 % of patients within 5 years; symptomatic ASD requiring surgery in 5–10 %.
- Mechanism: Fusion eliminates motion at one level, increasing stress on the discs above and below.
- Mitigation: Restoring global cervical lordosis, limiting the number of fused levels, and preserving facet joints during surgery help reduce ASD risk.
8. General Anesthesia–Related Risks
- Incidence: Comparable to any elective surgery.
- Considerations: Pulmonary complications, cardiac events, and postoperative nausea. Pre‑operative evaluation and optimized anesthesia protocols keep these complications low in the otherwise healthy cervical‑fusion population.
Balancing the Equation: Who Stands to Benefit Most?
Not every patient with neck pain is a candidate for ACF. Ideal candidates share several characteristics:
- Localized pathology confirmed on MRI or CT (e.g., single‑level disc herniation, osteophyte, or foraminal stenosis).
- Neurological compromise (radiculopathy, myelopathy) that correlates with imaging findings.
- Failure of at least 6–12 weeks of conservative care (physical therapy, analgesics, epidural steroid injections).
- Adequate bone quality to support graft and hardware; severe osteoporosis may necessitate alternative strategies (e.g., posterior fixation or vertebral body replacement).
- Absence of prohibitive medical comorbidities such as uncontrolled diabetes, active infection, or severe cardiopulmonary disease that would dramatically increase anesthesia risk.
For patients who meet these criteria, the probability of meaningful pain relief and functional improvement far outweighs the relatively low incidence of serious complications. Conversely, individuals with multilevel disease, diffuse cervical spondylosis, or significant comorbidities may benefit more from a posterior decompression, a motion‑preserving procedure such as cervical disc arthroplasty, or a non‑surgical regimen.
Mitigating Risks: Contemporary Surgical Strategies
Modern spine surgeons employ several tactics to minimize the complications listed above:
- Meticulous Soft‑Tissue Dissection – Use of a low‑profile retractor system with intermittent release reduces esophageal and RLN compression.
- Intra‑operative Neuromonitoring – Continuous somatosensory and motor evoked potentials alert the team to impending neural injury, often before irreversible damage occurs.
- Biologic Fusion Enhancers – Autograft, allograft, and osteo‑inductive agents augment bone healing, especially in smokers or older patients where fusion rates are otherwise lower.
- Optimized Implant Design – Low‑profile anterior plating systems and cages with teeth or porous surfaces lower screw pull‑out and cage subsidence rates.
- Post‑operative Protocols – Early mobilization combined with a brief (2–4 week) cervical collar in selected cases balances protection of the construct with rapid return to function.
- Pre‑habilitation – Strengthening the deep neck flexors and addressing modifiable risk factors (e.g., smoking cessation, glycemic control) before surgery has been shown to reduce infection and improve fusion outcomes.
The Recovery Journey: What to Expect
The typical postoperative timeline after a single‑level ACF proceeds as follows:
- Day 0–1: Observation in a recovery room; most patients are discharged home the same day or the next morning.
- Weeks 1–2: Light activity and neck range‑of‑motion exercises begin; many surgeons prescribe a soft‑diet if dysphagia is present.
- Weeks 3–6: Gradual increase in work‑related tasks; most office‑based jobs are cleared. Physical therapy focuses on strengthening and posture correction.
- Months 3–6: Radiographs confirm progressive bony bridging. Full activity, including sports that do not involve high‑impact cervical loading, is usually permitted.
- Year 1: Final assessment of fusion status (often via CT) and evaluation of long‑term symptom resolution.
Adherence to the prescribed rehabilitation plan, avoidance of heavy lifting (>10 lb) for at least 6 weeks, and maintenance of a neutral cervical posture are critical to maximizing the benefits of the fusion.
Bottom Line
Anterior cervical fusion srgery stands as a highly effective, evidence‑based solution for single‑level cervical radiculopathy and myelopathy that have not responded to conservative therapy. Its principal advantages—targeted decompression, reliable fusion, restoration of cervical alignment, rapid pain relief, and a relatively brief recovery—make it a first‑line surgical option for many patients. The most common drawbacks—transient dysphagia, hoarseness, and the potential for adjacent‑segment degeneration—are generally mild, predictable, and manageable when the surgeon follows contemporary best‑practice techniques. Serious complications such as vascular injury, permanent nerve damage, or deep infection are rare, especially in patients who are medically optimized and operated on by an experienced spine team.
When weighing the decision, patients should consider the severity of their neurological symptoms, the extent of radiographic disease, and their overall health profile. A thorough discussion with a spine surgeon, supplemented by imaging review and possibly second‑opinion consultation, will clarify whether the expected benefits of anterior cervical fusion justify its modest risks for any individual case. In the hands of skilled clinicians, ACF offers a high likelihood of durable relief, functional restoration, and an improved quality of life—an outcome that, for many, outweighs the manageable hazards inherent to any operative intervention.